Highlights

- “Kratom” commonly refers to an herbal substance that can produce opioid- and stimulant-like effects. Kratom and kratom-based products are currently legal and accessible in many areas, though U.S. and international agencies continue to review emerging evidence to inform kratom policy.1
- While there are no uses for kratom approved by the U.S. Food and Drug Administration, people report using kratom to manage drug withdrawal symptoms and cravings (especially related to opioid use), pain, fatigue and mental health problems.2,3,4 NIDA supports and conducts research to evaluate potential medicinal uses for kratom and related chemical compounds.
- NIDA also supports research towards better understanding the health and safety effects of kratom use. Rare but serious effects have been reported in people who use kratom, including psychiatric, cardiovascular, gastrointestinal and respiratory problems.1,5 Compared to deaths from other drugs, a very small number of deaths have been linked to kratom products and nearly all cases involved other drugs or contaminants.1,6,7,8,9,10
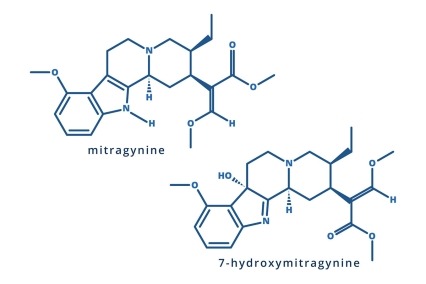
“Kratom” refers to both Mitragyna speciosa, a tree native to Southeast Asia, and to products derived from its leaves that are marketed as herbal supplements. Kratom leaves contain many chemical compounds (known as bioactive alkaloids) that can affect the body. The most well-studied compounds related to kratom are mitragynine and 7-hydroxymitragynine.1 (See How do kratom compounds work in the brain?)
Much is still unknown about chemical compounds related to kratom, the short- and long-term health and safety impacts of kratom use and kratom’s potential therapeutic uses. NIDA supports and conducts research on kratom and related chemical compounds to help inform kratom policy and health decision-making around kratom use. (See How is NIDA advancing research on about kratom?)
While kratom or its related compounds have not been approved by the U.S. Food and Drug Administration as safe and effective for any medical use, people report using kratom products to alleviate drug withdrawal symptoms and cravings (particularly for opioids), to alleviate pain and to help manage mental health problems.3,4,11,12,13,14,15,16 (See Why do people use kratom?) NIDA is particularly interested in studying how kratom use may impact opioid use, which continues to drive the drug overdose epidemic in the United States.
People typically use kratom by swallowing raw plant matter in capsule or powder form, mixing kratom powder into food or drinks, brewing the leaves as a tea, or taking liquid kratom extract.1 People who use kratom report both stimulant-like effects (increased energy, alertness and rapid heart rate) and effects that are similar to opioids and sedatives (relaxation, pain relief and confusion).10,17 Studies and case reports have also indicated rare adverse effects may be associated with kratom or individual kratom compounds.1,9 (See How does kratom affect the body?; Is kratom safe?)
Anthropologists report that kratom has been used in Southeast Asia for hundreds of years as a multi-purpose remedy in traditional medicine, to increase alertness and energy while working and during social gatherings.18 While estimates of the scope of kratom use in the United States vary,19 the expansion of kratom vendors and increasing case reports suggest kratom use has become more common over the past two decades.20
Researchers are still learning how kratom and kratom compounds affect the body, as well as how short- and long-term kratom use may impact health. While evidence is quickly evolving, early studies have revealed important information about how the drug works.
- Effects may vary widely. Like all drugs, kratom’s effects may depend on the amount taken, potency (concentration and strength), formulation of the product, the way it is ingested, other drugs in a person’s system, a person’s underlying medical conditions, and a person’s previous experience with the substance, among other factors.3, 4, 17 Importantly, kratom products vary, so effects are difficult to predict. Some kratom products have been found to contain contaminants that produce effects not associated with kratom or kratom compounds alone.6, 7, 21 Learn more: Is kratom safe?
- Kratom produces opioid- and stimulant-like effects. People who use kratom report both stimulant-like effects (increased energy, alertness and rapid heart rate) and effects that are similar to opioids and sedatives (relaxation, pain relief and confusion). While many people who use kratom report that smaller doses of kratom produce stimulant-like effects and larger doses produce opioid- or sedative-like effects,4 studies have not yet established that these effects depend on the amount or method of kratom consumed.10, 17
- Mitragynine, 7-hydroxymitragynine, and other kratom compounds drive these effects. The effect of kratom products can vary depending on the concentration and combination of specific kratom compounds within the product. While kratom leaves contain many chemical compounds that may influence the human body, the most well-studied is mitragynine. When ingested, mitragynine breaks down into another chemical called 7-hydroxymitragynine, which also influences the body and is an important subject of research.22 Learn more: How do kratom compounds work in the brain?
- Adverse effects range from mild to severe. Some people who use kratom have reported mild side effects, such as nausea, constipation, dizziness and drowsiness.3, 4 In case reports, clinicians report seeing patients with a wide range of rare but serious adverse effects associated with kratom exposure—including mental and neurological symptoms (confusion, tremors and seizures), heart and lung problems (high blood pressure and slow breathing), gastrointestinal problems (nausea and vomiting) and liver problems.1, 23 A very small number of deaths have been linked to kratom products, and nearly all cases involved other drugs or contaminants.1,6, 7, 8, 21, 24 (See Is kratom safe?)
- Drug interactions may influence effects. Studies suggest many people who use kratom also use other drugs and have conditions for which medications are often prescribed.3, 4, 17 Case reports suggest using kratom in combination with other drugs (sometimes called polysubstance use) may produce severe adverse effects, such as liver problems or even death.25 More research is needed to better understand the impact of using kratom in combination with other substances. (See Is kratom safe?)
- Long-term health effects are not well understood. Because kratom research is relatively new compared to more widely used drugs, there is little evidence to determine how kratom use may affect someone over time. Case reports do show regular, long-term, kratom use in large amounts may be associated with serious liver problems. These cases appear to occur unpredictably in a small minority of people who use kratom, and it is unclear what role other substances and underlying health conditions may play.9, 26 (See Is kratom safe?) Researchers are also still learning how often and to what extent people who use kratom experience withdrawal or substance use disorder symptoms related to kratom use. Learn more: Is kratom addictive? Do people experience kratom withdrawal?
- Research on potential therapeutic effects of kratom is ongoing. Researchers have not proven kratom to be safe or effective for any medical purpose, though kratom has been used in traditional medicine.18 Many people who use kratom products report doing so to self-treat pain, anxiety, depression, fatigue, and drug cravings and withdrawal symptoms (especially related to opioid use).1, 3 NIDA supports and conducts research on therapeutic uses of kratom and related compounds. Learn more: Could kratom be used as medicine?
Kratom leaves contain many chemical compounds (known as bioactive alkaloids) that influence the body. The most well-studied kratom-related compounds are mitragynine and 7-hydroxymitragynine (7-OH). Mitragynine is found in kratom leaves and breaks down into 7-OH in the body when digested.22, 27 Both activate mu-opioid receptors (specific molecular structures on the surface of nerve cells), but the resulting effects only partially compare to those of opioids like heroin or oxycodone.28
In general, neither kratom leaves nor mitragynine appear to lead to respiratory depression (trouble breathing) that is characteristic of a life-threatening opioid overdose. However, in laboratory models, 7-OH can cause respiratory depression that is reversed by naloxone. Even though the body converts mitragynine to 7-OH, this occurs slowly enough that it limits mitragynine’s effects on breathing.29 Scientists also have observed that mitragynine may bind to adrenergic receptors, serotonin receptors and dopamine receptors, which may be responsible for some of the arousing effects some people who use kratom report experiencing.1, 30, 31
Better understanding where and how kratom compounds work in the brain is an active area of NIDA-funded research. This basic research plays an important role in identifying kratom’s health effects and potential therapeutic uses. Learn more: How is NIDA advancing research on kratom?
Scientific research on kratom is relatively new compared to research on more widely used drugs. Much is still unknown about chemical compounds related to kratom, the short- and long-term health and safety impacts of kratom use and kratom’s potential therapeutic uses. In response to reports of increases in kratom exposures in the United States6 and emerging questions about kratom and its health effects, NIDA is supporting research on kratom’s use, effects, mechanisms and therapeutic potential.
To help inform kratom policy and health decision-making around kratom use, NIDA conducts and supports research on how kratom compounds work in the brain, as well as research on kratom use patterns, health effects, therapeutic uses and drug interactions. Because many people who use kratom also report using or previously using opioids and experiencing opioid use disorder, 2, 3 NIDA is particularly interested in studying how kratom use may impact opioid use, which has driven the drug overdose epidemic in the United States. Early studies have found that some people report using kratom to ease craving and withdrawal symptoms associated with other substances, including opioids and stimulants.5, 11, 13, 14, 15, 16
NIDA and the NIH HEAL (Helping to End Addiction Long-term®) Initiative are supporting several studies evaluating kratom and related compounds as potential treatments for chronic pain and for opioid withdrawal and opioid use disorder. One of these projects (also supported by the National Center for Advancing Translational Sciences and National Institute of Neurological Disorders and Stroke) includes efforts to help develop new medications, including kratom-derived products, as potential treatments for opioid use disorder.
NIDA also supports preclinical research to better understand how multiple kratom compounds produce complex pharmacological and behavioral effects, to evaluate kratom as a potential therapy for opioid use disorder and to investigate the chemistry and biology of kratom-derived compounds for their use as therapeutic drugs and as research tools. (See Could kratom be used as medicine?)
See more NIDA-funded projects related to kratom, and learn more about clinical trials involving kratom.
Among people aged 12 or older in 2021, an estimated 0.6% (or about 1.7 million people) reported using kratom in the past 12 months (2021 DT 8.22).*
Source: 2021 National Survey on Drug Use and Health**
* Estimates of how many people regularly use kratom vary.19
** The COVID-19 pandemic had an impact on data collection for the 2021 National Survey on Drug Use and Health (NSDUH). For more information, please see the 2021 NSDUH Frequently Asked Questions from the Substance Abuse and Mental Health Services Administration.
NIDA conducts and supports research to better understand the diverse reasons people use kratom.3 Kratom has been used in its native Southeast Asia for centuries to produce opioid- and stimulant-like effects, including increased energy and relaxation.18 (See How does kratom affect the body?)
In recent years, studies suggest people across the globe use kratom for these and many other reasons.1, 3, 4 Researchers have found that people report using kratom to alleviate pain, to address symptoms of mental health conditions like anxiety and depression, to help stop or reduce opioid or other substance use and to manage withdrawal symptoms and cravings related to opioids and other drugs. Most report multiple reasons for using kratom.3, 11, 32
While research is underway to explore possible therapeutic benefits (see Could kratom be used as medicine?), kratom products have not been demonstrated to be safe and effective for any medical condition. Of note, safe and effective medications are approved to help control withdrawal symptoms and cravings associated with opioid use disorder, as well as other substance use disorders. Learn more about pain treatment from the NIH Pain Consortium and about mental health treatment from the National Institute of Mental Health.
U.S. and international agencies have expressed concern that kratom products may cause serious harm.1 There are no uses for kratom approved by the U.S. Food and Drug Administration (FDA), and the FDA has warned consumers not to use kratom products because of potential adverse effects.
The FDA, the U.S. Centers for Disease Control and Prevention and NIDA support and conduct research to measure and better understand the short- and long-term safety risks of kratom use and inform policy around kratom regulation.
Currently, several safety issues related to kratom have been identified:
- Kratom products may contain harmful contaminants. There are no uses for kratom approved by the FDA, and kratom products have been found to contain contaminants that produce effects not associated with kratom or kratom compounds alone, including heavy metals and harmful bacteria.1, 6, 7, 8, 21 Of note, researchers and regulators have found similar instances of contamination in many other products marketed as herbal supplements.33, 34 Read more about supplement regulation from the FDA.
- Adverse effects range from mild to severe. Some people who use kratom have reported mild side effects, such as nausea, constipation, dizziness and drowsiness.3, 4 In case reports, clinicians report seeing patients with a wide range of very rare but serious adverse effects associated with kratom exposure—including mental and neurological symptoms (confusion, tremors and seizures), heart and lung problems (high blood pressure and slow breathing), gastrointestinal problems (nausea and vomiting) and liver problems.1, 23 Researchers continue to study potential adverse effects in humans, animal models and cells, including possible damage to the cardiovascular system.10, 23, 35 (See How does kratom affect the body?)
- A very small number of deaths have been linked to kratom products compared to deaths from other drugs.1, 6, 7, 8, 24 While more research is needed, it appears that fatal overdose from kratom use alone is extremely rare. A 2019 report found that 11 deaths between 2011 and 2017 in the United States were associated with kratom exposure, including two deaths associated with kratom exposure alone.6 In contrast, during that same period, more than 200,000 people died from opioid-related overdose.36
- Drug interactions may influence effects. Studies suggest many people who use kratom also use other drugs and have conditions for which medications are often prescribed,3, 4, 17 and case reports suggest polysubstance use (the use of multiple drugs) involving kratom has been associated with severe adverse effects, such as death and liver problems.25 More research is needed in this area to assess the safety of using kratom in combination with other substances.
- Long-term health and safety effects are not well understood. Because kratom research is relatively new compared to research on more widely used drugs, there is little evidence to determine how kratom use may affect someone over time. Case reports do show regular, long-term, kratom use in large amounts may be associated with serious liver problems. These cases appear to occur unpredictably in a small minority of people who use kratom, and it is unclear what role other substances and underlying health conditions may play.9, 26
- Effects on pregnancy are not well understood. Very little research is available on kratom use before, during and after pregnancy, but there have been reports of opioid-like neonatal abstinence syndrome in infants born to women who regularly use kratom.37 Learn more: How does kratom use affect pregnancy?
- Safety effects of intoxication are not well understood. The impact of kratom intoxication (taking enough to be impaired) on driving, operating heavy machinery, or performing other tasks that could be dangerous if impaired has not been extensively studied.9, 38, 39
Learn more about kratom and safety from the FDA.
Very little research is available on kratom use before, during and after pregnancy. A 2021 report suggests that many cases of kratom use during pregnancy likely also involve the use of other substances, and the effects of kratom alone on pregnancy are difficult to determine without further research. The same report identified at least five cases of opioid-like neonatal abstinence syndrome in infants born to women who regularly used kratom but not opioids. The infants in these cases all responded well to standard treatments given to infants experiencing neonatal abstinence syndrome related to opioids.37
NIDA conducts and supports research to better understand how often and to what extent people who use kratom experience withdrawal and substance use disorder symptoms related to kratom use.
To be diagnosed with a substance use disorder, a person must meet specific diagnostic criteria for continued, compulsive substance use despite negative consequences. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5)—a reference text published by the American Psychiatric Association that health professionals use to diagnose substance use disorders and other psychiatric disorders—does not include a specific diagnosis related to kratom use.40 However, some researchers studying kratom have modified criteria to study kratom use patterns and symptoms that resemble other substance use disorders.3
Studies suggest people may experience mild to moderate withdrawal symptoms when they stop regular kratom use,41, 42 but more research is needed to understand to what extent people develop substance use disorder symptoms related to kratom.1, 3, 9
Preliminary data from anonymous surveys of people who use kratom suggest a minority of people report experiencing kratom-related withdrawal symptoms and a smaller minority report experiencing substance use disorder symptoms related to kratom use.3
Some experts are concerned about kratom’s addictive potential because the main kratom compounds, mitragynine and 7-hydroxymitragynine, partially activate the same receptors (specific molecular structures on the surface of nerve cells) in the brain on which drugs with known addictive properties act. However, researchers have observed that the way kratom compounds activate these receptors may reduce the potential for addiction relative to opioids.28, 29, 30, 31 Further, studies in animal models indicate that the addictive potential of mitragynine and 7-hydroxymitragynine may differ from one another.43 Further research is needed to better understand how various compounds related to kratom interact to influence the risk of withdrawal and addiction. (See How do kratom compounds work in the brain?)
While withdrawal and substance use disorder symptoms related to kratom use have not been extensively studied, some people who use kratom report experiencing them.1, 3, 9 (See Is kratom addictive? Do people experience kratom withdrawal?) There are currently no approved medical therapies for these conditions. In very limited cases, some researchers have reported using medications44, 45, 46 and other therapies47 to address withdrawal and substance use disorder symptoms related to kratom use41 in humans and animal models—though robust clinical trials are still needed to evaluate these and other experimental treatment options.
See more information on seeking substance use treatment and other medical attention.
NIDA and other institutes at NIH support and conduct research to evaluate potential medicinal uses for kratom and kratom compounds. While kratom has not been proven safe or effective for any medical purpose, kratom has been used in traditional medicine in some countries,1, 18 and many people who use kratom report doing so to self-medicate for pain, anxiety, depression, substance use disorders and substance withdrawal.1, 3, 11 Studies in animal models suggest kratom and related compounds potentially have other therapeutic properties, such as antidepressant and pain-relieving properties, that may warrant further study.1, 48
Of particular interest to NIDA, early studies suggest kratom and kratom compounds warrant further study as experimental treatments for substance use disorders, specifically opioid use disorder.9, 48 Such treatments are urgently needed to help curb the drug overdose epidemic in the United States. NIDA and its partners conduct and support research evaluating kratom and related compounds as potential treatments for chronic pain and for opioid withdrawal and opioid use disorder. Learn more: How is NIDA advancing research on kratom?
While kratom use or sale has been banned or restricted in several countries,9 kratom products are currently legal and accessible online49 and in stores in many areas of the United States. The U.S. Drug Enforcement Administration (DEA) has listed kratom as a “drug of concern,” though kratom and kratom compounds are not listed on the U.S. schedule of controlled substances.
In 2021, the World Health Organization’s (WHO) Expert Committee on Drug Dependence (ECDD) examined the evidence on kratom’s health effects and concluded that there is insufficient evidence of adverse effects that would warrant additional critical review or inclusion in the United Nations list of internationally controlled substances. (See the full WHO ECDD report on kratom.) Kratom remains on the list of substances under surveillance by the WHO ECDD.
Learn more about kratom and its legal status in the United States from the Drug Enforcement Administration (DEA).
Find More Resources on Kratom
- Learn more about kratom regulation and safety from the U.S. Food and Drug Administration (FDA).
- Learn more about kratom and its legal status from the Drug Enforcement Administration (DEA).
- Learn more about kratom products marketed as herbal supplements from the National Institutes of Health (NIH) National Center for Complementary and Integrative Health (NCCIH).
- United Nations, Commission on Narcotic Drugs. Summary of assessments, findings and recommendations of the 44th World Health Organization’s (WHO) Expert Committee on Drug Dependence (ECDD), 11–15 October 2021. Vienna; 9-10 December 2021. Report No. E/CN.7/2021/CRP.12 [1]
- Palamar JJ. Past-year kratom use in the U.S.: Estimates from a nationally representative sample. Am J Prev Med. 2021;61(2):240-245. doi:10.1016/j.amepre.2021.02.004 [2]
- Garcia-Romeu A, Cox DJ, Smith KE, Dunn KE, Griffiths RR. Kratom (Mitragyna speciosa): User demographics, use patterns, and implications for the opioid epidemic. Drug Alcohol Depend. 2020;208:107849. doi:10.1016/j.drugalcdep.2020.107849 [3]
- Grundmann O. Patterns of Kratom use and health impact in the US-Results from an online survey. Drug Alcohol Depend. 2017;176:63-70. doi:10.1016/j.drugalcdep.2017.03.007 [4]
- Leong Bin Abdullah MFI, Singh D. The adverse cardiovascular effects and cardiotoxicity of kratom (Mitragyna speciosa korth.): A comprehensive review. Front Pharmacol. 2021;12:726003. Published 2021 Sep 27. doi:10.3389/fphar.2021.726003 [5]
- Post S, Spiller HA, Chounthirath T, Smith GA. Kratom exposures reported to United States poison control centers: 2011-2017. Clin Toxicol (Phila). 2019;57(10):847-854. doi:10.1080/15563650.2019.1569236 [6]
- Kronstrand R, Roman M, Thelander G, Eriksson A. Unintentional fatal intoxications with mitragynine and O-desmethyltramadol from the herbal blend Krypton. J Anal Toxicol. 2011;35(4):242-247. doi:10.1093/anatox/35.4.242 [7]
- Henningfield JE, Grundmann O, Babin JK, Fant RV, Wang DW, Cone EJ. Risk of death associated with kratom use compared to opioids. Prev Med. 2019;128:105851. doi:10.1016/j.ypmed.2019.105851 [8]
- United Nations, Expert Committee on Drug Dependence. Pre-review report: Kratom (Mytragyna speciosa), mitragynine, and 7-hydroxymitragynine. 11–15 October 2021. Geneva. [9]
- Leong Bin Abdullah MFI, Singh D, Swogger MT, Rahim AA, Vicknasingam B. The prevalence of psychotic symptoms in kratom (Mitragyna speciosa korth) users in Malaysia. Asian J Psychiatr. 2019;43:197-201. doi:10.1016/j.ajp.2019.07.008 [10]
- Smith KE, Rogers JM, Schriefer D, Grundmann O. Therapeutic benefit with caveats?: Analyzing social media data to understand the complexities of kratom use. Drug Alcohol Depend. 2021;226:108879. doi:10.1016/j.drugalcdep.2021.108879 [11]
- Singh D, Narayanan S, Vicknasingam B, et al. The use of kratom (Mitragyna speciosa korth) among people who co-use heroin and methamphetamine in Malaysia. J Addict Med. 2021;10.1097/ADM.0000000000000876. doi:10.1097/ADM.0000000000000876 [12]
- Vicknasingam B, Narayanan S, Beng GT, Mansor SM. The informal use of ketum (Mitragyna speciosa) for opioid withdrawal in the northern states of peninsular Malaysia and implications for drug substitution therapy. Int J Drug Policy. 2010;21(4):283-288. doi:10.1016/j.drugpo.2009.12.003 [13]
- Saref A, Suraya S, Singh D, et al. Self-Report Data on regular consumption of illicit drugs and HIV risk behaviors after kratom (Mitragyna Speciosa korth) initiation among illicit drug users in Malaysia. J Psychoactive Drugs. 2020;52(2):138-144. doi:10.1080/02791072.2019.1686553 [14]
- Smith KE, Lawson T. Prevalence and motivations for kratom use in a sample of substance users enrolled in a residential treatment program. Drug Alcohol Depend. 2017;180:340-348. doi:10.1016/j.drugalcdep.2017.08.034 [15]
- Boyer EW, Babu KM, Macalino GE. Self-treatment of opioid withdrawal with a dietary supplement, kratom. Am J Addict. 2007;16(5):352-356. doi:10.1080/10550490701525368 [16]
- Singh D, Narayanan S, Grundmann O, Dzulkapli EB, Vicknasingam B. Effects of Kratom (Mitragyna Speciosa korth) use in regular users. Subst Use Misuse. 2019;54(14):2284-2289. doi:10.1080/10826084.2019.1645178 [17]
- Cinosi E, Martinotti G, Simonato P, et al. Following "the roots" of kratom (Mitragyna speciosa): The evolution of an enhancer from a traditional use to increase work and productivity in southeast Asia to a recreational psychoactive drug in western countries. Biomed Res Int. 2015;2015:968786. doi:10.1155/2015/968786 [18]
- Henningfield JE, Grundmann O, Garcia-Romeu A, Swogger MT. We need better estimates of kratom use prevalence. Am J Prev Med. 2022;62(1):132-133. doi:10.1016/j.amepre.2021.07.022 [19]
- Prozialeck WC, Jivan JK, Andurkar SV. Pharmacology of kratom: an emerging botanical agent with stimulant, analgesic and opioid-like effects. J Am Osteopath Assoc. 2012;112(12):792-799. [20]
- Dixon RB, Waggoner D, Davis M, Rembold K, Dasgupta A. Contamination of some kratom products with Salmonella. Ann Clin Lab Sci. 2019;49(5):675-677. [21]
- Eastlack SC, Cornett EM, Kaye AD. Kratom-pharmacology, clinical implications, and outlook: A comprehensive review. Pain Ther. 2020;9(1):55-69. doi:10.1007/s40122-020-00151-x [22]
- Graves JM, Dilley JA, Terpak L, et al. Kratom exposures among older adults reported to U.S. poison centers, 2014-2019. J Am Geriatr Soc. 2021;69(8):2176-2184. doi:10.1111/jgs.17326 [23]
- Eggleston W, Stoppacher R, Suen K, Marraffa JM, Nelson LS. Kratom use and toxicities in the United States. Pharmacotherapy. 2019;39(7):775-777. doi:10.1002/phar.2280 [24]
- Veltri C, Grundmann O. Current perspectives on the impact of Kratom use. Subst Abuse Rehabil. 2019;10:23-31. Published 2019 Jul 1. doi:10.2147/SAR.S164261 [25]
- Schimmel J, Dart RC. Kratom (Mitragyna speciosa) liver injury: A comprehensive review. Drugs. 2020;80(3):263-283. doi:10.1007/s40265-019-01242-6 [26]
- Kruegel AC, Uprety R, Grinnell SG, et al. 7-Hydroxymitragynine is an active metabolite of mitragynine and a key mediator of its analgesic effects. ACS Cent Sci. 2019;5(6):992-1001. doi:10.1021/acscentsci.9b00141 [27]
- Kruegel AC, Gassaway MM, Kapoor A, et al. Synthetic and receptor signaling explorations of the mitragyna alkaloids: Mitragynine as an atypical molecular framework for opioid receptor modulators. J Am Chem Soc. 2016;138(21):6754-6764. doi:10.1021/jacs.6b00360 [28]
- Hill R, Kruegel AC, Javitch JA, et al. The respiratory depressant effects of mitragynine are limited by its conversion to 7‐OH mitragynine. Br J Pharmacol. 2022; 179(14):3875-3885. doi:10.1111/bph.15832
Zuarth Gonzalez JD, Ragsdale AK, Mukhopadhyay S, et al. Mitragynine and 7-hydroxymitragynine: Bidirectional effects on breathing in rats. J Pharmacol. Exp. Ther. 2025, 392(11):103720. doi:10.1016/j.jpet.2025.103720 - Matsumoto K, Mizowaki M, Suchitra T, Murakami Y, Takayama H, Sakai S, et al. Central antinociceptive effects of mitragynine in mice: contribution of descending noradrenergic and serotonergic systems. Eur J Pharmacol. 1996;317(1):75–81. [30]
- Hanapi NA, Chear NJ, Azizi J, Yusof SR. Kratom alkaloids: Interactions with enzymes, receptors, and cellular barriers. Front Pharmacol. 2021;12:751656. Published 2021 Nov 17. doi:10.3389/fphar.2021.751656 [31]
- Coe MA, Pillitteri JL, Sembower MA, Gerlach KK, Henningfield JE. Kratom as a substitute for opioids: Results from an online survey. Drug Alcohol Depend. 2019;202:24-32. doi:10.1016/j.drugalcdep.2019.05.005 [32]
- Charen E, Harbord N. Toxicity of herbs, vitamins, and supplements. Adv Chronic Kidney Dis. 2020;27(1):67-71. doi:10.1053/j.ackd.2019.08.003 [33]
- Hudson A, Lopez E, Almalki AJ, Roe AL, Calderón AI. A review of the toxicity of compounds found in herbal dietary supplements. Planta Med. 2018;84(9-10):613-626. doi:10.1055/a-0605-3786 [34]
- Lu J, Wei H, Wu J, et al. Evaluation of the cardiotoxicity of mitragynine and its analogues using human induced pluripotent stem cell-derived cardiomyocytes. PLoS One. 2014;9(12):e115648. Published 2014 Dec 23. doi:10.1371/journal.pone.0115648 [35]
- CDC WONDER. Multiple Cause of Death 1999-2020. Centers for Disease Control and Prevention, National Center on Health Statistics. Released December 2021. Accessed January 2022. [36]
- Wright ME, Ginsberg C, Parkison AM, Dubose M, Sherbondy M, Shores E. Outcomes of mothers and newborns to prenatal exposure to kratom: a systematic review. J Perinatol. 2021;41(6):1236-1243. doi:10.1038/s41372-021-00952-8 [37]
- Papsun DM, Chan-Hosokawa A, Friederich L, Brower J, Graf K, Logan B. The trouble with kratom: Analytical and interpretative issues involving mitragynine. J Anal Toxicol. 2019;43(8):615-629. doi:10.1093/jat/bkz064 [38]
- Veltri C, Grundmann O. Association of kratom use with impairment: Many legal questions remain. J Anal Toxicol. 2019;43(5):e8-e9. doi:10.1093/jat/bkz012 [39]
- American Psychiatric Association. Substance-related and addictive disorders. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington D.C.: 2013. doi:10.1176/appi.books.9780890425596.dsm16 [40]
- Stanciu CN, Gnanasegaram SA, Ahmed S, Penders T. Kratom withdrawal: A systematic review with case series. J Psychoactive Drugs. 2019;51(1):12-18. doi:10.1080/02791072.2018.1562133 [41]
- Singh D, Narayanan S, Vicknasingam BK, et al. Severity of pain and sleep problems during kratom (Mitragyna speciosa korth) cessation among regular kratom users. J Psychoactive Drugs. 2018;50(3):266-274. doi:10.1080/02791072.2018.1443234 [42]
- Hemby SE, McIntosh S, Leon F, Cutler SJ, McCurdy CR. Abuse liability and therapeutic potential of the Mitragyna speciosa (kratom) alkaloids mitragynine and 7-hydroxymitragynine. Addict Biol. 2019;24(5):874-885. doi:10.1111/adb.12639 [43]
- Khazaeli A, Jerry JM, Vazirian M. Treatment of kratom withdrawal and addiction With buprenorphine. J Addict Med. 2018;12(6):493-495. doi:10.1097/ADM.0000000000000435 [44]
- Vento AE, de Persis S, De Filippis S, et al. Case report: Treatment of kratom use disorder with a classical tricyclic antidepressant. Front Psychiatry. 2021;12:640218. Published 2021 Mar 31. doi:10.3389/fpsyt.2021.640218 [45]
- Hassan R, Sreenivasan S, Müller CP, Hassan Z. Methadone, buprenorphine, and clonidine attenuate mitragynine withdrawal in rats. Front Pharmacol. 2021;12:708019. Published 2021 Jul 12. doi:10.3389/fphar.2021.708019 [46]
- Kalin S, Dakhlalla S, Bhardwaj S. Treatment for kratom abuse in a contingency-management-based MAT setting: A case series. J Opioid Manag. 2020;16(5):391-394. doi:10.5055/jom.2020.0594 [47]
- Grundmann O, Brown PN, Henningfield J, Swogger M, Walsh Z. The therapeutic potential of kratom. Addiction. 2018;113(10):1951-1953. doi:10.1111/add.14371 [48]
- Williams RS, Nikitin D. The internet market for kratom, an opioid alternative and variably legal recreational drug. Int J Drug Policy. 2020;78:102715. doi:10.1016/j.drugpo.2020.102715 [49]