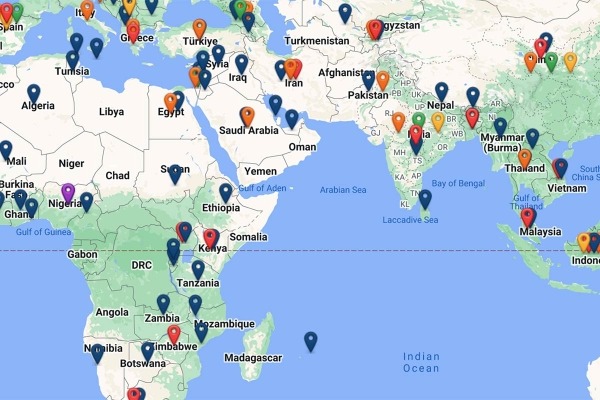
The NIDA International Program builds partnerships among individual scientists, research institutions, and national and international organizations to:
- Promote international research collaboration
- Sponsor research training fellowships
- Exchange information on addiction science
About Us or Email: ip@nida.nih.gov